We use our phones for just about everything so why use them to diagnose cancer?
Smartphones tell the the weather, read out traffic conditions and instantly connect people from around the world, but now app developers are claiming that mobile phones can diagnose skin cancer.
A study published in the Medical Journal of Australia by senior research fellow at the Queensland University School of Public Health, Monika Janda and Chair of Queensland University’s Dermatology Research Centre, Dr Peter Soyer, found the accuracy and reliability of ‘melanoma early detection’ apps can range from 6 per cent to over 98 per cent.
“There are many different apps out there and they offer a vast variety of quality of service, so we need to be aware of these differences and people need to inform themselves of what the app can or cannot provide.”
“People need to treat these apps as they would any other technology – critically reflect on the pros and cons for themselves and think about exactly how they want to use it and why,” Janda says.
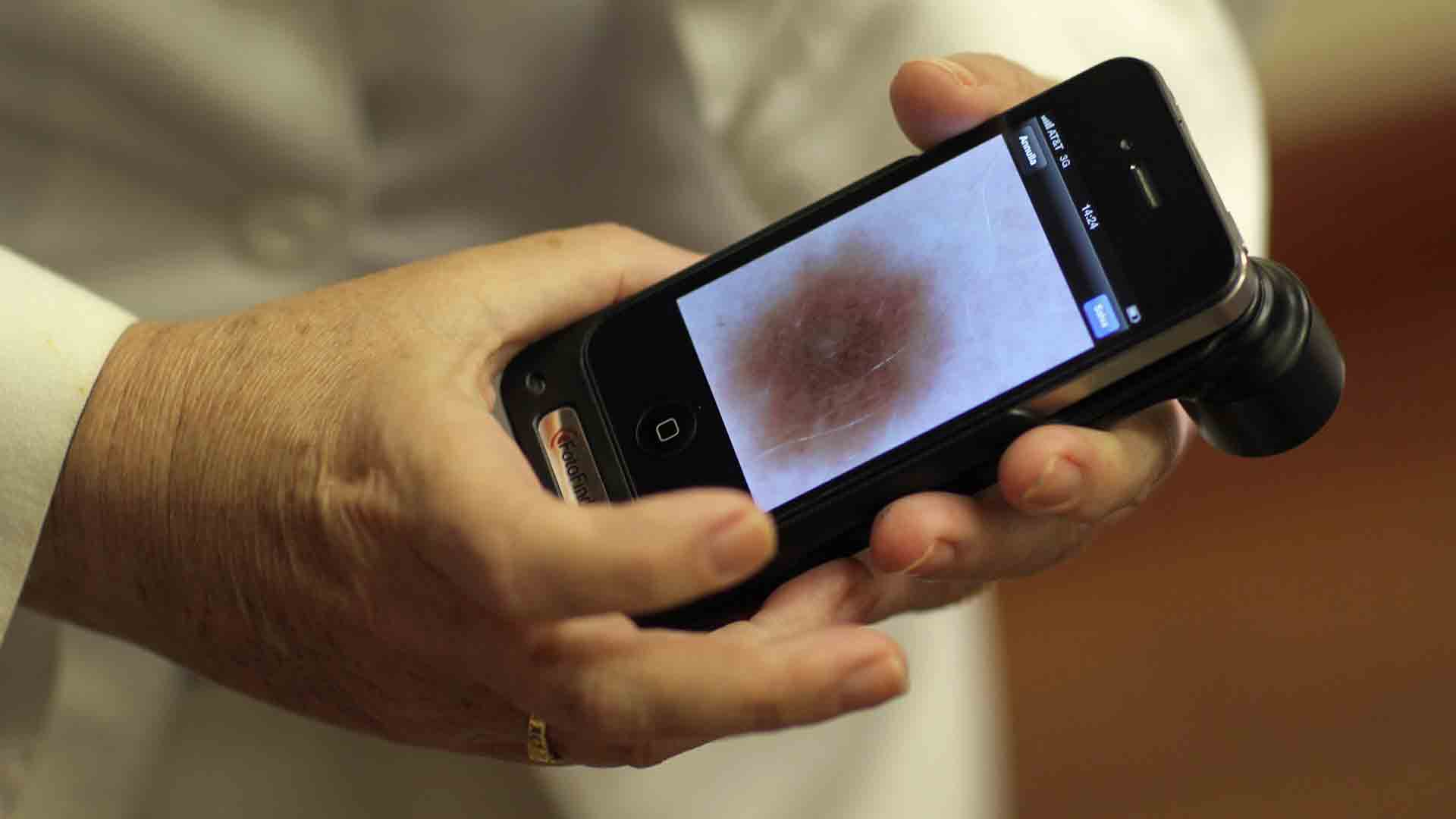
While government guidelines for the use of ‘medical’ apps are non-existent in Australia, the Dermatology Research Centre and the University of Queensland are providing research participants with a magnifying device for their smartphone as part of a trial of the technology. The device is able to target specific lesions on the body with a polarised light that returns a clear picture and allows the app to provide a brief description of the shape, colour, development and history of the mark.
The app that had the highest level of accuracy sent the image directly to a board-certified dermatologist for analysis. However, Associate Professor Dr Stephen Schumack, President of the Australasian College of Dermatologists and consultant dermatologist at Sydney’s Royal North Shore Hospital says it is to early to endorse any skin cancer detection smartphone apps.
“While there is some evidence that apps that take standardised pictures and transmit them to a dermatologist for reporting might be more accurate, there are still so many variables between actually taking the photo and a dermatologist then interpreting the information,” Schumack says.
“The equipment that is used to take the photo, who the photo was taken by, which app was used and the lighting and angle of the photo may all effect the reliability of the process.”
Despite a five-year survival rate of 90 per cent for men and 94 per cent for women, more than 2000 Australians died from skin cancer in 2011. While local doctors have over 1 million consultations per year for skin cancer, Dr Janda believes skin cancer detection apps have the potential to boost patient-doctor interactions and provide more accessible ways for people to engage with their health care professionals.
“These apps could engage more people and get them to take a more active role in the health of their skin. It is likely that doctors will increasingly use apps in their practice, or will be asked about results received through such apps by their patients.”
However, Skin Cancer Prevention Manager at the NSW Cancer Council, Vanessa Rock, warns against relying on apps to detect skin cancer.
“The biggest worry would be apps with low sensitivity submitting poor images for analysis. Melanoma has a high cure rate if detected and treated early. However, a melanoma that is misdiagnosed and not treated appropriately can move to other parts of the body such as the liver or brain and can become fatal,” Rock says.
While there are hopes further studies will lead to more accurate and reliable skin cancer detection apps, the Therapeutic Goods Administration and the NSW Cancer Council are yet to endorse or approve any mobile app that claims to detect skin cancer.